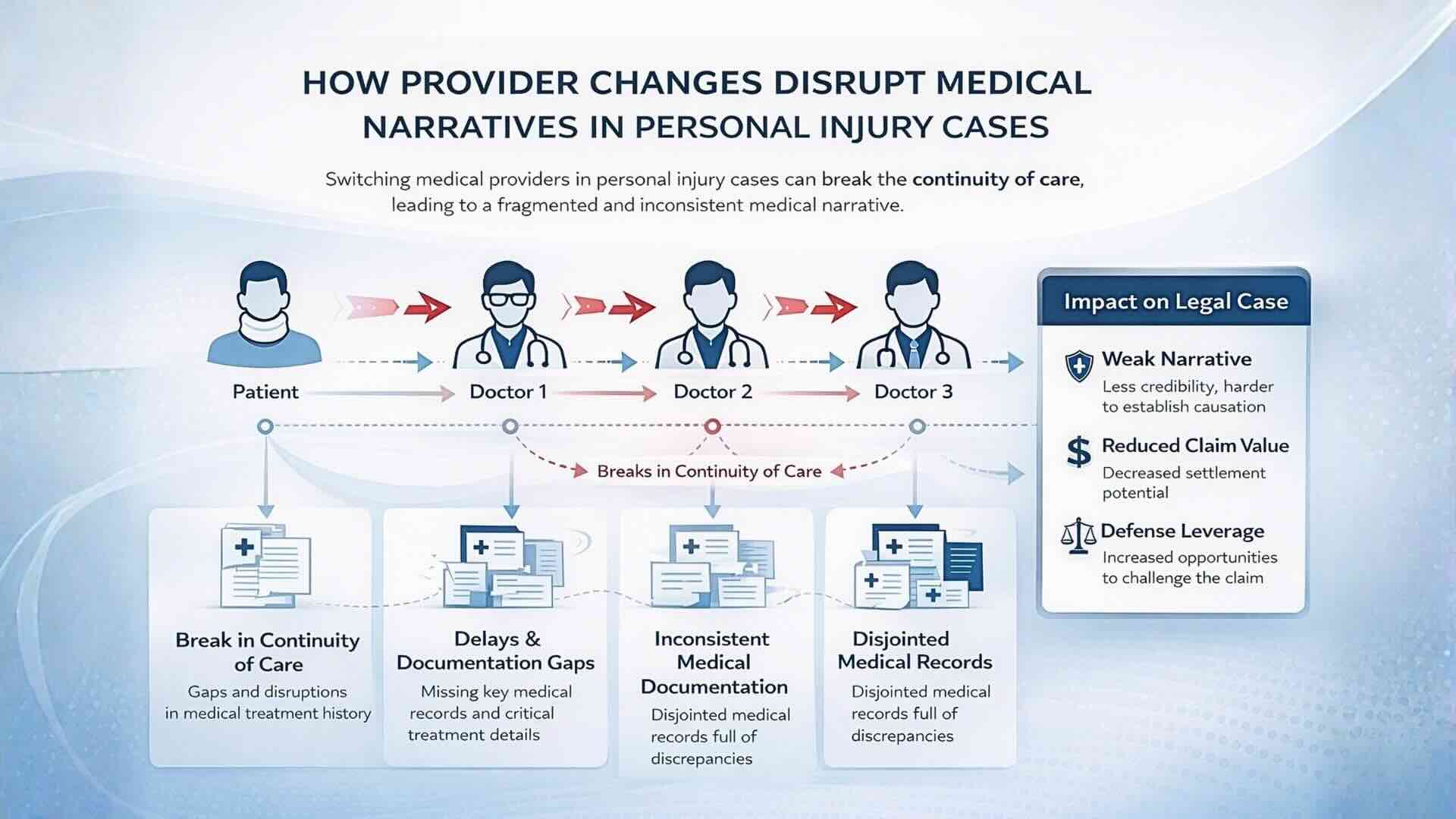
In personal injury litigation, the outcome often depends on how clearly the medical record tells the story of the injury. Many cases lose strength not because the injury is minor, but because the documentation becomes inconsistent over time. One of the most underestimated drivers of this breakdown is provider changes in personal injury cases.
When patients move between multiple providers, even for legitimate reasons, the medical narrative often begins to lose structure. Instead of presenting a clear progression, records may reflect subtle inconsistencies, missing context, or shifts in clinical interpretation. On their own, these issues may seem minor, but over time they make it harder to prove causation, damages, and long-term impact.
Claims involving multiple treating providers are often examined more closely when causation is under review. In many of those cases, the provider changes end up influencing how the claim is judged almost as much as the injury itself.
Why Medical Narratives Matter More Than Most Realize
A personal injury case is more than a series of appointments; it is a medical narrative that must be supported by clear clinical evidence. That narrative must clearly explain three things: what happened, how the injury developed, and how it continues to affect the patient.
When documentation is consistent, the record forms a clear and credible timeline. It establishes a baseline, tracks symptom progression, and supports causation. However, when changing medical providers in PI cases happens repeatedly, that continuity starts to break down.
Instead of showing continuity, the record may begin to reflect unexplained differences. Pain levels shift, diagnoses evolve, and treatment direction changes without clear linkage. This is where inconsistent treatment providers injury claims begin to lose credibility, even when the injury itself is valid.
A Real-World Scenario: Where Narratives Break Down
A common treatment sequence shows how this problem develops. A patient is first evaluated in an emergency setting, then transitions to a chiropractor, and later receives care from a specialist.
At each stage, documentation reflects a different clinical focus:
- Initial provider documents acute strain with limited functional impact.
- Second provider emphasizes structural dysfunction and mobility issues.
- Third provider records chronic pain with possible neurological involvement.
None of these entries are necessarily wrong on their own. The problem is that they do not align cleanly when viewed together.
In cases involving provider changes, this variation often creates a fragmented narrative. The injury appears to evolve inconsistently, which introduces doubt about causation and severity. From a defense perspective, this makes it easier to argue that the condition may not be fully related to the accident.
How Provider Changes Disrupt Medical Continuity
When provider changes in personal injury cases occur, the disruption is rarely caused by a single issue. Instead, it develops through multiple layers of inconsistency that gradually weaken the medical narrative. These disruptions often affect how symptoms are documented, how treatment is spaced over time, and how clinical context is preserved between providers. Understanding these patterns is critical, because even small breakdowns in continuity can significantly impact how a claim is evaluated.
Subtle Documentation Misalignment
When patients change providers in PI cases, the most damaging inconsistencies are often subtle rather than obvious.
Common examples include differences in:
- pain scale reporting (e.g., moderate vs. severe)
- onset language (sudden vs. gradual)
- functional limitations (restricted vs. tolerable)
Individually, these differences may seem minor. But once they appear across multiple providers, they often create a pattern that weakens the overall narrative. In inconsistent treatment providers injury claims, these small contradictions are often used to challenge credibility.
Timeline Fragmentation and Treatment Gaps
Another major problem caused by provider changes in personal injury cases is disruption in treatment continuity.
Even short gaps between providers can alter how a case is perceived. From a legal standpoint, inconsistent timing may suggest that symptoms are not persistent or not severe.
Even brief interruptions in care can affect how continuity is viewed in contested cases, especially when the treatment history is already fragmented. Over time, these gaps make it harder to demonstrate a clear and uninterrupted progression of symptoms.
Loss of Clinical Context Between Providers
When patients transition between providers, prior records are not always fully integrated into the new provider’s assessment.
Key details such as the mechanism of injury, earlier symptom patterns, and initial diagnostic findings may not be carried consistently from one provider to the next.
In treatment history disruption in injury cases, this creates a fragmented record where continuity is implied rather than documented. From a litigation standpoint, implied continuity is far less persuasive than continuity that is clearly documented.
How Insurance Companies Systematically Use These Gaps
In claims involving provider changes in personal injury cases, adjusters often review the records closely for alignment problems.
Their evaluation typically centers on three areas:
- consistency of symptom reporting across providers.
- continuity of treatment timelines.
- alignment of diagnosis with the original mechanism of injury.
When discrepancies appear in these areas, insurers often use them to argue that the condition is unrelated, exaggerated, or tied to pre-existing factors. In many inconsistent treatment providers injury claims, the defense strategy focuses on documentation breakdown rather than medical validity.
For a deeper look at how these problems develop, see our article on medical record inconsistencies in PI cases.
The Hidden Impact on Causation
Causation usually does not collapse all at once; it weakens gradually as inconsistencies build. When provider changes in personal injury cases disrupt documentation, the connection between incident and injury becomes less defined.
A fragmented timeline makes it difficult to show continuity. Variations in language create uncertainty about symptom progression. Over time, this allows opposing parties to introduce alternative explanations.
In cases involving treatment history disruption in injury cases, insurers often argue that the condition developed independently or followed a natural progression unrelated to the incident. Once this argument is introduced, it becomes significantly harder to maintain claim value.
Why Provider Changes Happen and Why That’s Not the Real Issue
Changing medical providers in PI cases is often unavoidable. Patients move between providers due to referrals, insurance limitations, or access to specialized care.
However, in a legal setting, the key issue is not why the provider changed, but whether the documentation remained consistent.
Even well-justified transitions can lead to inconsistent treatment providers injury claims if documentation is not aligned. The issue is not the act of changing providers, but the absence of structured continuity across those changes.
What Most Legal Teams Miss
One reality many legal teams underestimate is this:
Most documentation issues are not caused by major errors they are caused by a lack of coordination over time.
Claims are often weakened not by the injury itself, but by how it is managed across multiple providers. While each provider may document accurately within their own scope, the absence of a unified structure creates a fragmented narrative.
Many legal teams focus heavily on injury severity but overlook the importance of maintaining alignment across providers. Without active oversight, inconsistencies do not just appear they build gradually.
By the time these issues are recognized, they are often already influencing negotiations and shaping claim value.
A Practical Framework to Control Provider-Related Risk
Managing provider changes in personal injury cases requires more than collecting records; it requires a structured and proactive system.
An effective control system includes:
- building a unified timeline that integrates all providers into a single narrative.
- standardizing terminology to minimize contradictions across records.
- explicitly documenting the reason for every provider transition.
This approach helps turn fragmented records into a coherent narrative and reduce the damage that changing medical providers in PI cases can cause, especially in complex claims involving multiple phases of treatment.
Strengthening Case Integrity Through Structured Review
Consistency rarely happens on its own; it usually requires deliberate organization and review.
Using professional medical record review helps identify inconsistencies early, address gaps, and keep the narrative aligned across providers.
This is especially critical in cases involving treatment history disruption in injury cases, where multiple transitions increase the risk of narrative breakdown.
The Role of Medical-Legal Coordination
As cases become more complex, coordination between medical and legal teams becomes essential.
Specialized medical-legal professionals can reconstruct fragmented timelines, identify inconsistencies before they are challenged, and strengthen the documentation used to support causation.
If your firm is handling cases affected by multiple provider changes, speak with our team about building a more consistent medical-legal process.
Conclusion
Provider changes in personal injury cases are often treated as a minor logistical issue, even though they can directly shape how a claim is evaluated.
When documentation becomes fragmented, the medical narrative weakens, and so does the ability to defend causation and damages. On the other hand, when records are aligned and transitions are properly managed, even complex cases can remain strong.
In personal injury litigation, success is rarely determined by what happened alone. It depends on how clearly and consistently that story is documented from start to finish.